Since most of the malformations occur on the face, PWS is a clinically significant problem in the great majority of patients. PWS should not be considered a cosmetic problem but a disease with potentially devastating psychological and physical complications. Detailed studies have documented lower self-esteem and problems with interpersonal relations in PWS patients.
The cause and origin of PWS remains incompletely uncovered. It is believed that PWS develop within the first 2-8 weeks of gestation.
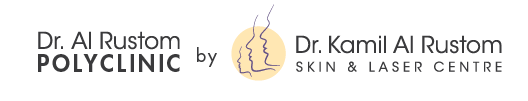
PWS is a progressive vascular malformation of the skin that remains throughout life and there is no involution. PWS are well demarcated and flat and grow proportionately in surface area with the child. In infants and young children, PWS are flat red macules. However, the lesions tend to darken progressively to purple and, by adult age, often become raised as a result of the development of vascular papules or nodules. These changes in color and contour are attributed to progressive ectasia of the abnormal dermal vascular plexus. Over time, blood vessels become more dilated and susceptible to spontaneous bleeding or hemorrhage following minor trauma. Bleeding can be difficult to control, necessitate hospitalization and may also increase the likelihood of skin infection. If left untreated, PWS often become incompatible with normal life due to the development of vascular nodules on the skin surface which can often bleed spontaneously with incidental trauma.
The pulsed dye laser in conjunction with cryogen spray cooling (“dynamic cooling device” or “DCD”) is now the treatment of choice for PWS. Yellow light produced by the pulsed dye laser penetrates up to 2 mm into the skin and is preferentially absorbed by hemoglobin within the dilated PWS blood vessels. The heat within the vessel lumen causes blood vessel damage which is evidenced by intense purpura (“bruised” appearance of the skin). Several treatment sessions spaced at 4-8 week intervals are required for maximum efficacy. The number of treatments required for maximum PWS fading can be variable and unpredictable. Treatment side effects are mainly limited to post-operative swelling and purpura, which generally resolves within 2 weeks. With the addition of cryogen spray cooling, the risks of scarring or changes in the normal skin pigmentation are minimal after pulsed dye laser therapy performed by an experienced physician.